It starts like a cramp, it lingers like a bruise, it tightens like a vise. You flex your foot and the pain bites back. Night hits and your calf throbs, warm, swollen, shiny, like it’s not yours. You call it a strain—cute—but that ache won’t quit. Long flight? Surgery? Hormones? Sitting all day? Keep guessing if you like. Or face the one sign you can’t ignore next.
Key Takeaways
- Deep, persistent calf or thigh ache that doesn’t ease with stretching or rubbing.
- Cramp-like pain that lingers, worsens with movement or foot flexion, often worse at night.
- One-sided swelling with tight, warm, glossy skin; calf looks bigger than the other.
- Tenderness and stubborn muscle tightness or pulling; throbbing or tugging discomfort may mislead.
- If in doubt, get a duplex ultrasound—imaging confirms; don’t rely on pain or swelling alone.
How a DVT Feels: Common Sensations in the Calf or Thigh

Usually it starts like a cramp that won’t shut up. You rub it. You stretch. It laughs. The feeling digs in, a deep ache that won’t bargain, not today. Then comes the pull, that stubborn muscle tightness that says don’t move—so you move. It pushes back. Hard. Walking feels wrong. Flex your foot and it snaps back with a nasty reminder. Sit still and it broods, heavy, sullen, plotting. You keep asking, sore or something worse? Your calf whispers, guess again. Pain migrates, not far, just enough to mess with your head. It throbs, it tugs, it nags, again and again. Night makes it louder. You bargain with water and willpower. Cute. This pain wants attention. Yours. Now. Stand up, it follows, sit, seethes.
Visible and Physical Signs to Watch For
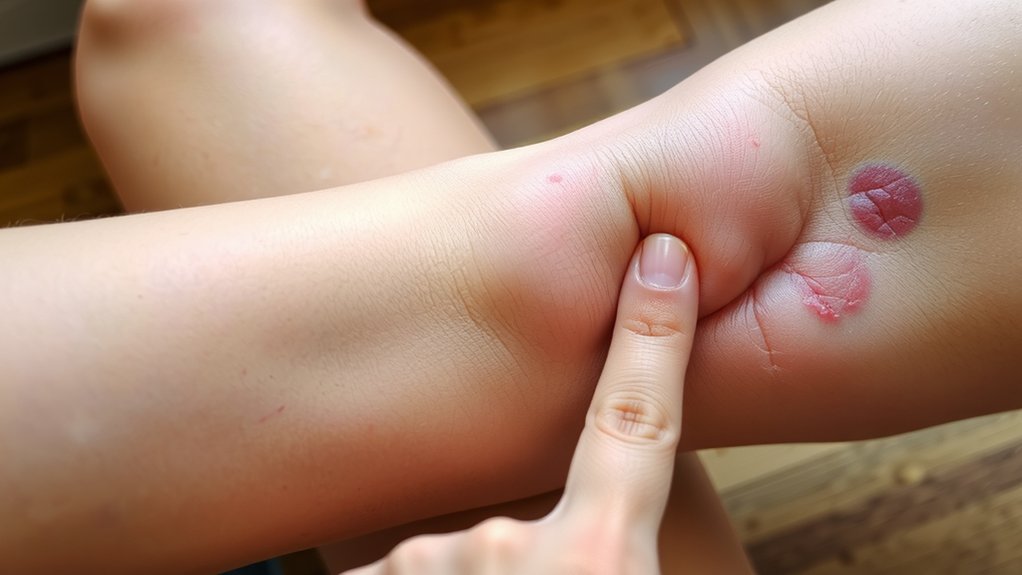
Pain picks a fight, then your skin joins in. You see swelling that’s not shy—one calf looks pumped, the other looks lazy. The skin feels tight, glossy, almost plastic. Touch it. It’s warm, hotter than the other leg, like it’s hoarding heat. Now the color show: skin discoloration that shifts from red to purple to blue, not cute, not normal. Press a thumb; the dent lingers. That’s your cue. Veins speak too. prominent veins snake across the surface, louder, thicker, stubborn. They weren’t there yesterday. They’re bragging today. Walking hurts. Flex your foot and the calf snaps back with attitude. Socks leave angry tracks. Ankles balloon by night. And if tingling or numbness sneaks in, stop guessing and act. Call it out. Move fast.
When Leg Pain Is Likely Not a Clot

While clots love drama, most leg aches don’t. Your calf screams after sprints? That’s a muscle strain, not a crisis. Pain pops with a step then fades when you stop. It flares when you stretch the exact spot. You can point to it. Bullseye. Heat helps. Massage helps. You move and it loosens. That’s not a clot, that’s mileage.
Electric stabs shooting down the leg? Think nerve compression, not a silent killer. Sit weird, get zapped, stand up, it chills. Pins and needles gatecrash then ghost. Classic. Cramps wake you at 2 a.m., you flex, they quit. Bruise on the shin, tender as truth, but superficial. Achy joints bark after stairs, then hush. Consistent rhythm. Predictable pain. No swelling circus. No sudden, spreading doom.
Risk Factors That Raise Your Chances
Because you sit still for hours, your blood plots against you. But immobility isn’t the whole story. Genes load the gun. Inherited thrombophilia makes your clotting switch too reactive, too fast. Family history? That’s your neon warning. Age adds friction. Extra weight squeezes veins and slows flow. Cancer and its treatments crank clotting up. So does pregnancy. And let’s talk hormones. Hormonal contraceptives and hormone therapy tilt the balance toward sludge. Smoke on top of that? You’re stacking dynamite. Prior DVT or PE? Your body remembers—and not in a cute way. Heart failure, kidney disease, inflammatory disorders, all push the scale. You’re not helpless. Ask about testing. Cut the risks you own. Pick movement. Hydrate. Challenge the assumptions. Now. Start today. No excuses. Ever.
Triggers and Situations That Precede DVT

You sit still for hours on a plane or the couch and tell yourself it’s harmless—it’s not. Blood slows, legs swell, and a clot can set up shop before you even stand—still think that’s nothing? Had recent surgery or a hard hit—tissue damage lights the fuse and a DVT shows up grinning, so you move, hydrate, and speak up fast.
Prolonged Immobility Risks
Although the chair looks innocent, it can turn your legs into a slow‑motion traffic jam. Sit long. Blood pools. Valves get lazy. Clots lurk while you scroll and snack. You think you’re resting. You’re not. You’re training your veins to stall. Hours in a car, a binge‑watch, a desk grind—same trap. Your calves stop pumping. Need a wake‑up? Imagine pressure ulcers and bone loss riding shotgun with that clot risk. Stand every hour. March in place. Flex. Set a ruthless timer. Move when it screams. Not later. Plane ride? Road trip? Work marathon? You don’t need gear. You need movement, now.
| Situation | Risk | Move Now |
|---|---|---|
| Sitting 2+ hours | High | Stand, calf raises |
| Long flights | Higher | Aisle laps, water |
| Road trips | High | Pit stops, stretch |
Recent Surgery or Trauma
Surgery and injuries flip your clot switch. You just cut flesh, stirred inflammation, and slowed blood flow. Perfect storm. During incision healing, your body dumps clotting signals like confetti. Useful at the wound. Deadly in a calf vein. Scar formation stiffens tissues, you limp, you sit, you stall. Blood pools. It plots. Anesthesia knocked you out; bed rest kept you there. Casts squeeze. IV lines jab. Dehydration thickens the mix. You think that’s harmless? Tell your swollen, hot leg. Tell that sudden cramp that won’t quit. That’s not “just recovery.” That’s a siren. Move. Hydrate. Ask about stockings and blood thinners. Demand a walk, today, not tomorrow. Hate pain? Then don’t baby the limb. Respect it, yes. But keep the river flowing. Right now.
Warning Signs of a Pulmonary Embolism
How do you tell a harmless gasp from a lung-clogging emergency?
Your body shouts. You feel sudden breathlessness like the air got thinner and meaner. A rapid heartbeat kicks like it’s late for class. Chest pain? Sharp, stabbing, worse when you inhale or cough, like a nail under the rib. You cough, maybe streaks of blood—yeah, that drama. You turn clammy, sweaty, pale, or lips shade blue. Dizzy rush hits, lights dim, knees plot a collapse. Anxiety spikes out of nowhere—alarm without a fire. Breathing stays fast and shallow; you can’t “walk it off.” One calf? It’s swollen, warm, tender, the sneaky backstory. Climb stairs and your lungs riot. Lie still and it doesn’t quit. That’s the tell. The problem moves; your oxygen doesn’t.
When to Seek Urgent Medical Care
When do you stop guessing and call for help? When your calf balloons, burns, or turns hot and tight. When one leg swells, not both. When pain spikes while you walk, then throbs at rest. When skin blushes red or purple and the veins pop like a roadmap. Don’t bargain. Don’t ice it and wait.
If breath runs short, chest clenches, heart races, or you faint, forget pride. That’s 911. Now.
Use triage guidelines like a checklist, not a horoscope. Single‑sided swelling? Sudden pain? New warmth? Check check check. You don’t need perfect certainty. You need speed.
No ride? Use telehealth access for instant direction, but aim for ER, not a lullaby. Tell them your leg changed fast. Demand urgency. You’re not overreacting today.
Diagnosis, Treatment, and Prevention Basics
You want answers not guesswork—so you get a leg ultrasound, maybe a D‑dimer, because swollen calves don’t lie. If it’s DVT you don’t wait and see—you start blood thinners fast, sometimes clot busters or a filter, because lungs aren’t optional. Prevention is blunt—move on flights, hydrate, wear compression socks, quit smoking—because you’d rather walk tomorrow than roll the dice today.
DVT Diagnostic Tests
Stop guessing—prove it. You want answers, not vibes. Start with a D‑dimer. Low risk plus a negative test? Walk away confident—because D dimer accuracy is high for ruling out clots, not confirming them. High risk or red‑flag symptoms? You need imaging. The Ultrasound technique—compression duplex—shows the vein refuse to collapse. That’s your smoking gun. Still fuzzy? Repeat scans or escalate. CT venography? Rare, but real. And no, Google doesn’t count.
| Test | What it shows | Use it when |
|---|---|---|
| D‑dimer | Fibrin fragments | Low to moderate risk, rule‑out |
| Compression ultrasound | Noncompressible vein | Most first-line cases |
| CT/MR venography | Filling defects | Complex anatomy or unclear ultrasound |
Still doubt it? Then stop stalling and get tested today. Pain lies. Swelling lies. Imaging doesn’t. Your leg, your call. Choose proof. Now.
Treatment and Prevention
Proof beats fear—now fix it. You’ve got a clot or a scare, so act. Anticoagulants thin the chaos and prevent bigger trouble. Take them exactly as prescribed. No cowboy doses. Medication adherence isn’t cute, it’s survival. Miss pills, spin the roulette. Hit every dose, stack the odds.
Move. Walk like you mean it. Sit forever, pay later. Wear Compression stockings if your clinician says so; they squeeze, you win. Elevate the leg. Hydrate. Stop smoking. Drop extra weight. Hate these orders? Fine, negotiate with gravity and clots instead.
Know red flags. Sudden chest pain, breathlessness, coughing blood—don’t Google, call emergency. Follow-up matters. Blood tests, imaging, plan tweaks. Ask dumb questions loudly. Travel smart. Stand, stretch, repeat. Prevention isn’t magic. It’s discipline, today. Do it.