You want the truth about a new knee? It looks swollen, bandaged, and a little scary. The incision runs straight and tight, shiny like plastic, itchy like crazy. Bruises slide down your calf. X‑rays? Metal meets plastic, neat and unapologetic. Your leg lines up straighter. Your walk starts to change. Pain shifts, then backs off. But what’s normal—and what should make you call fast? Let’s push into that now.
Key Takeaways
- On the outside: a midline scar over the knee, with early swelling and bruising that fade as the scar flattens and lightens over months.
- On X‑ray: bright metal femoral cap and tibial tray; the plastic spacer looks dark; you may see screws and thin cement lines.
- Desired alignment: a straight hip‑knee‑ankle line, level tibial baseplate, appropriate posterior slope on lateral view, and midline patellar tracking.
- Warning X‑ray signs: progressive radiolucent halos, component subsidence, varus/valgus tilt, eccentric liner wear, and bone loss under the tray.
- Typical timeline: tight, bulky look initially; swelling eases by 2–6 weeks; scar matures by months; overall contour normalizes over 3–12 months.
What You’ll See Right After Surgery
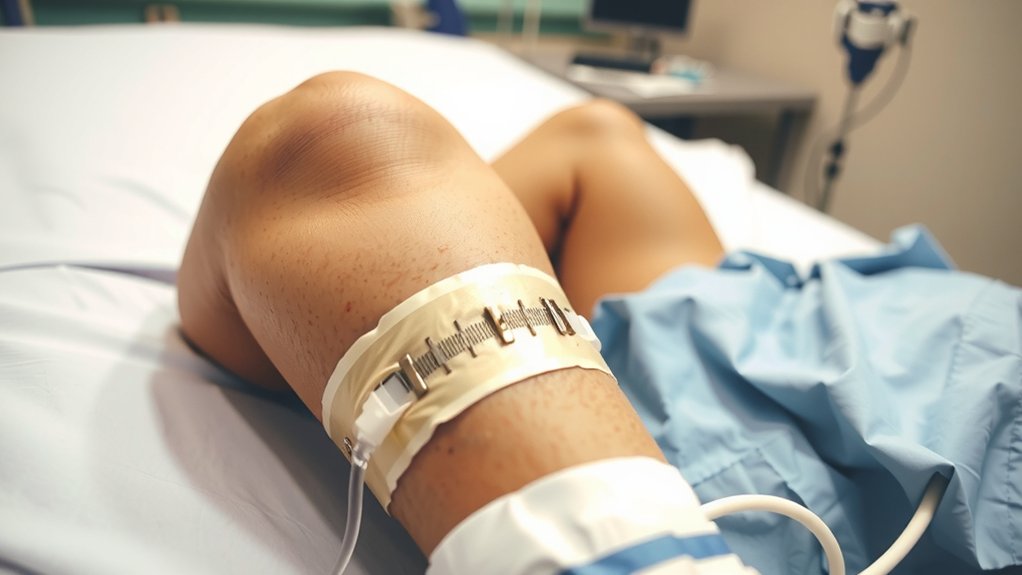
Even before the anesthesia fades, here’s the deal—you’ll wake up to a bandaged, bulky knee that looks like it lost a fight and somehow won. Your leg feels huge. Heavy. Numb, maybe burning, thank the anesthesia effects and the nerve block tag team. You hear beeps. You’re wired to monitoring devices like a borrowed science project—pulse ox on your finger, cuff on your arm, leads on your chest. Glamorous? Please. You’ve also got an IV pole that follows like a clingy friend. An ice sleeve hugs the knee hard. Compression boots squeeze your calves, rhythmically, like bossy mitts. You’ll test the knee sooner than you think. You’ll stand with a walker. You’ll curse. Then you’ll breathe, focus, and move. Because forward. Now. Do it.
Incisions, Scars, and Skin Changes
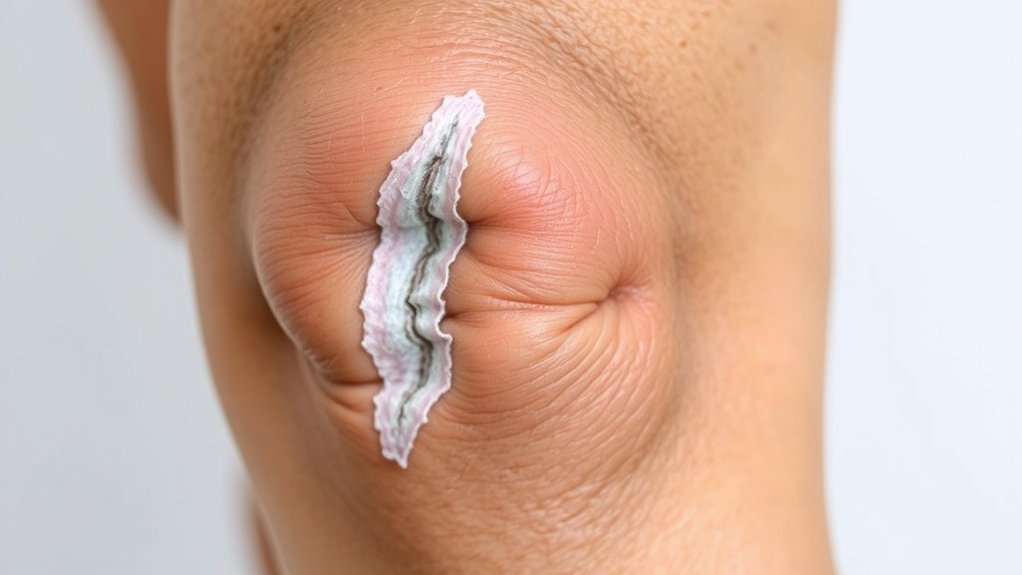
While the metal hides inside, the proof sits on your skin—front and center. That incision is no whisper. It runs straight down the knee like a bold underline. You’ll call it a badge. Or a billboard. It starts tight, shiny, and bossy. It itches. It pulls. It dares you to bend.
You want smooth? Too late. Scars remodel. They pale, flatten, thicken, or misbehave. Hair may skip the line. Skin may feel numb on one side, electric on the other. Weird? Yes. Wrong? No.
Swelling, Bruising, and How They Resolve

The scar shouts, but the swelling screams. You wake, look down, and think, balloon animal. Yep, your knee. Fluid rushes in, nerves complain, skin looks tight as a drum. Bruising slides downhill into the calf and ankle. Gravity wins. You ice, elevate, compress. You move, gently, because motion pumps. That’s the engine. Hematoma resolution starts ugly, then fades like a bad rumor. Colors change. Purple to green to yellow to gone. Meanwhile, lymphatic remodeling gets to work, building better drains, slower than you want, faster than you fear. Two weeks, less pressure. Six weeks, slimmer. Three months, you almost forget—until you overdo it. Boom, puff city. Don’t panic. Reset. Feet up. Cold pack. Breathe. Tomorrow fights back. So do you. Stronger knee, calmer skin.
How the Implant Looks on X-Rays
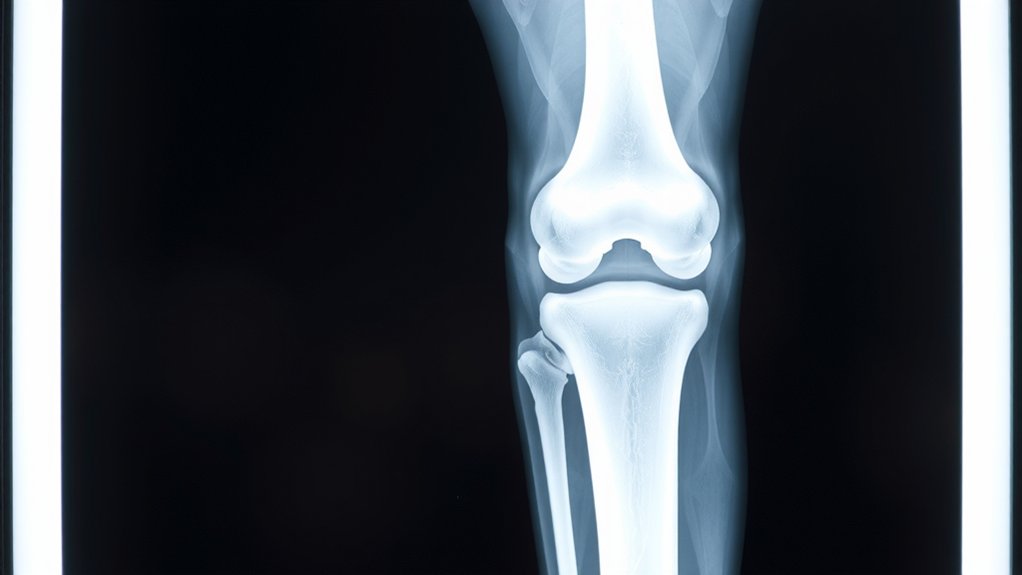
On the X-ray you’ll spot the metal femur cap, the tibial tray, maybe screws or cement lines, while the plastic spacer plays hide-and-seek because it’s mostly invisible. They should line up like soldiers—straight joint line, centered parts, patella tracking true—not crooked, not tilted, not “good enough.” See dark gaps, shifting edges, screw creep, or bone getting eaten away; that screams loosening and wear, and yes you call your surgeon now, not later.
Visible Components on Radiographs
X‑ray film doesn’t lie. You see the metal first: the bright femoral cap hugging the thighbone, the tibial baseplate like a shiny tray, maybe a stem plunging deeper. The plastic insert? It mostly disappears, a shadow gap that fools amateurs, not you. A round patellar button can glare back. Cement shows up as a pale cuff. Screws look like tiny drill bits daring you to blink. You want clarity, not guesswork, so you demand radiation safety and clean technique. Because blur isn’t mystery. It’s failure. Watch for image artifacts—buttons, zippers, motion streaks—that pretend to be problems. Don’t buy the illusion. Ask for sharp edges, balanced contrast, honest exposure, minimal noise. You paid for parts you can actually see, today. No excuses. Show the metal.
Alignment and Positioning Signs
You stared at metal; now you judge it. On the AP view, draw the hip‑knee‑ankle line. It should slice straight through the center of the femoral and tibial components. No lazy varus, no smug valgus. The tibial baseplate sits level to the joint line, with an even rim. On the lateral, you want controlled posterior slope, not a ski jump. Femoral component hugs the distal contour and stays parallel; the box isn’t tilted. Patella tracks midline, not sulking lateral. Pegs and keel look centered, not flirting with cortex. Rotation? Symmetric condylar shadows, equal overhang, clean trochlear groove. Compare limbs: gait symmetry starts here; stance width stops lying. If the metal lines up, you walk straighter. If it doesn’t, you feel it. Every single step.
Loosening and Wear Indicators
When pain lingers, the pictures snitch. X‑rays don’t lie; you hate that. Look for sneaky gaps around the metal. Radiolucent halos. Growing? That screams loosening. The cement line should be crisp; fuzz means trouble. Edges bite into bone? Good. Edges drifting? Bad. You’ll also spot bone resorption nibbling under the tray. That shadow isn’t “nothing.” It’s warning lights.
Now wear. Polyethylene thins. The joint space shrinks. Debris triggers swelling and, yeah, metal ions can spike with certain alloys. Feel hot, stiff, weak after steps? Don’t shrug. Demand comparisons. Today.
| Sign | What you see | Why it matters |
|---|---|---|
| Progressive halo | Darker rim | Micromotion |
| Subsidence | Component sinks | Instability |
| Varus tilt | Lopsided line | Overload |
| Eccentric wear | Uneven space | Liner loss |
Get images, compare angles, crush doubt, move now.
Alignment and Leg Shape Before vs. After
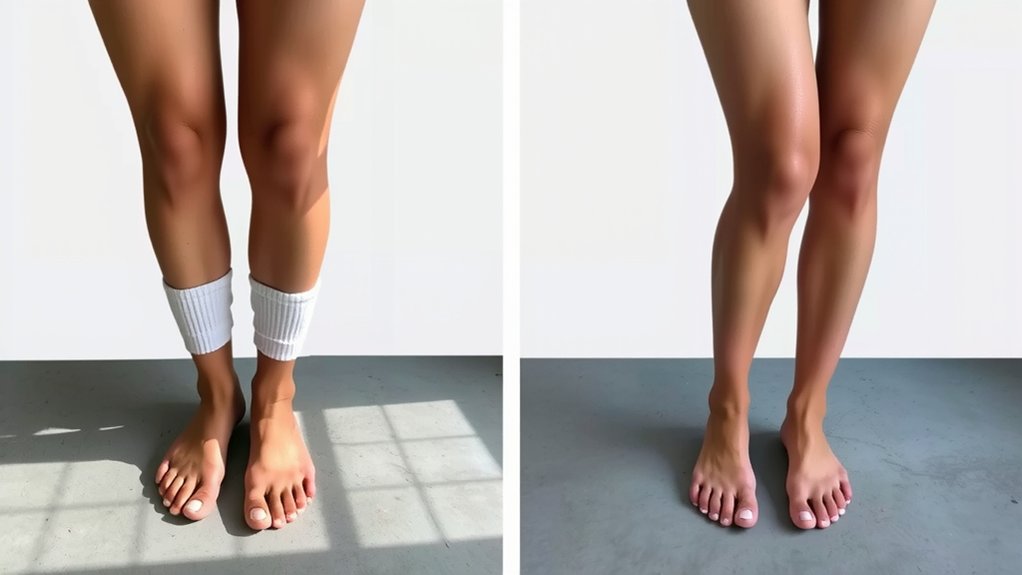
Although that crooked leg felt “normal” to you, the mission after knee replacement is brutal and simple—straighten the limb and line it up so it carries weight like it should. Before surgery, you leaned, twisted, and cheated. Varus, valgus, whatever label—your knee drifted. Your thigh rotated. Your foot shouted. After surgery, the bones obey. The joint tracks. You stand taller. Hips stop arguing. Ankles stop panicking. That’s alignment. It’s math, not vibes. With a straighter frame, gait symmetry finally shows up. Steps match. Stride evens. You don’t lurch like a pirate. Now muscle balance matters. Quads fire. Glutes steer. Calf finishes. You own the line. Not the brace. Not the cane. You. Straight, centered, unapologetic. Walk forward. Keep it straight. Own every step today.
What Feels Normal vs. Warning Signs
How do you tell if that ache is fine or a five‑alarm? You listen hard and stop making excuses. Mild soreness after activity? Normal. Heat that fades? Normal. A steady throb at rest that spikes at night? Not cute. Track your Pain patterns. Predictable ups after stairs beat random stabs while you’re sitting. Clicks without pain? Whatever. Grinding with a catch? Nope.
Now your radar: Sensory changes. A small numb zone near the scar happens. Spreading numbness, pins and needles with weakness, burning that crawls up the leg? That’s a siren. Swelling that softens by evening? Fine. A tight balloon with shiny skin, angry redness, or funky drainage? Call. Short breath, calf pain, sudden pop, fever, chills. Don’t wait. Don’t bargain. Act. Do it.
Recovery Timeline and Milestones
Three phases. Early, weeks 0–2. You stand, you shuffle, you swear. Swelling nags. Pain barks. You bend to 90 degrees and lock the quad because yes, control matters. Then weeks 3–6. You ditch the walker, maybe the cane, and hit real strength milestones: 0–110 flexion, straighter gait, one flight of stairs without a drama soundtrack. Finally weeks 7–12 and beyond. You drive, you shop, you work, you forget the brace you never liked. Long arc? Six to twelve months for solid endurance and trust, sometimes longer. Now the punchline: emotional recovery doesn’t follow a calendar. Some days you’re a champion. Some days you sulk. That’s normal. Count wins. Note setbacks. Keep the clock honest. Demand progress. Refuse excuses. Move. Own the pace. Nothing passive.
Tips to Support Healing and Cosmetic Results
You want a clean scar and a knee that doesn’t pout—then stop guessing and nail your wound care, starting today. Wash your hands, change dressings on schedule, keep the incision dry and boring, and call out redness, gunk, or fever like a fire alarm—no excuses. Then play offense: silicone sheets, sunscreen like you’re hiding from the sun, gentle massage when your surgeon clears it, and no heroic picking because you’re not a scab archaeologist.
Wound Care Essentials
After the surgery, the real fight starts at the incision. Baby it. But don’t baby yourself. Wash hands like you mean it. Keep the dressing clean dry intact. Use moisture barriers for showers, not wishful thinking. Change dressings as ordered, not when you feel lucky. Red streaks, foul odor, thick drainage? Call. Elevate to reduce throb, ice to tame heat, and move as cleared. Blood thinners onboard? Expect oozing, not a flood. Don’t pick. Don’t peek. You’re not a detective. Bag used supplies; practice safe dressing disposal. Surface wipe faster. Sleep like it’s your job. Your knee will reward discipline, and punish shortcuts. Stay sharp. Your choice. Right now.
| Action | When | Why |
|---|---|---|
| Wash hands | Before touch | Kill germs |
| Change dressing | As ordered | Control moisture |
Scar Minimization Strategies
Incision behaving? Good. Don’t get cocky. You want a thinner, flatter line, not a raised road. Start simple. Hands off scabs. Keep it clean and dry until cleared. Then silicone gel or sheets daily. They work. Massage the line when healed, slow and firm for a few minutes. Reduce tension with paper tape during activity. Sun? Block it hard. SPF 50 or long sleeves. Hydrate, eat protein, vitamin C, quit smoking. Move the knee, don’t grind the scar.
Now the head game. Scar psychology matters. Stop doom-scrolling close‑ups. Track progress weekly, not hourly. Ask your surgeon about lasers or microneedling later.
Check Insurance coverage for silicone, PT, even counseling. Humor helps. So does patience. You’re building a badge, not a billboard. Own that knee.