Like a plot twist you didn’t ask for, you spot a lump under your skin and panic—don’t. A typical lipoma feels soft and rubbery, slides under your fingers, looks smooth‑edged, not angry red, sometimes with little veins draped over it. It grows slow, pea to plum, usually painless. So relax? Not so fast. Hard, fixed, fast‑growing, or painful means a different story. You want the quick checks, the smart call, and the plan—now.
Key Takeaways
- Soft, rubbery, doughy lump under normal-looking skin; smooth, round or oval with clear edges.
- Usually painless, non-tender, not warm; skin color unchanged, sometimes veins visible over the bulge.
- Freely mobile under the skin—slides sideways with pressure and springs back.
- Grows slowly over months to years; typical size ranges from pea to plum.
- Hard, fixed, rapidly enlarging, or painful lumps with redness or ulceration are not typical—see a clinician.
What a Lipoma Looks Like on the Skin
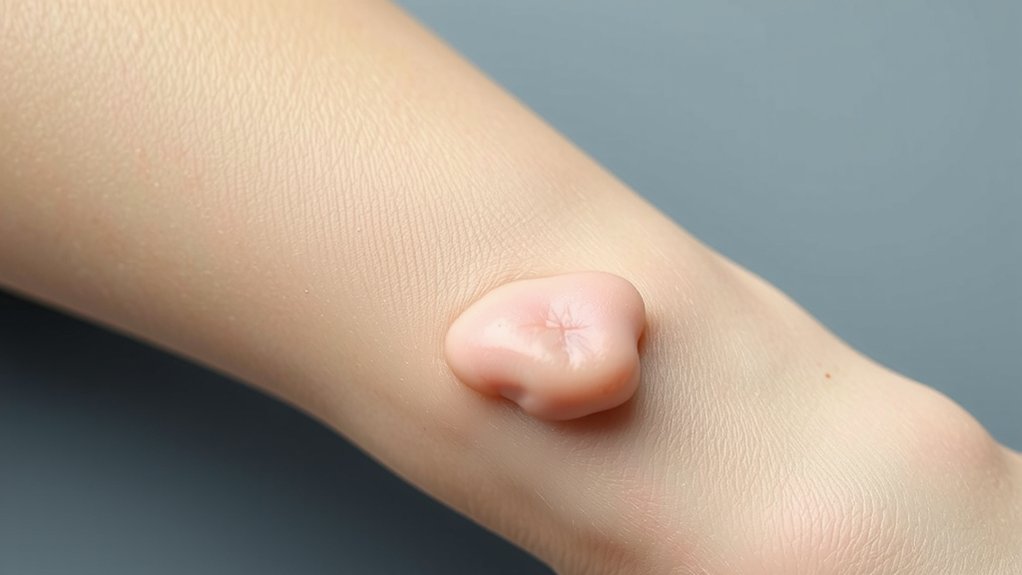
Although the name sounds scary, a lipoma looks like exactly what it is: a soft, squishy lump under your skin that minds its own business. You see a smooth hill rise under otherwise normal skin. Not jagged. Not angry. Just there. Roundish, maybe oval, with edges that don’t pick a fight. The skin coloration? Usually unchanged. No raging reds or villainous purples, just your usual tone over a subtle bulge. Sometimes you’ll notice prominent veins stretched a bit by the curve. Relax. That’s physics, not panic. It grows slow, like a procrastinator on a couch. Weeks. Months. Boring. You want drama? Wrong tumor. It keeps its outline neat and predictable. No crusts. No sores. No surprise eruptions. See it. Snort. Move on. Carry on.
How a Lipoma Feels: Texture, Firmness, and Mobility
How does it actually feel? You press, it pushes back. Not hard like a marble. Not mush like jelly. A lipoma gives that rubbery feel, springy yet calm. You poke it again. It slides. It dodges. It moves under your fingers like a lazy puck, then settles. You squeeze the edge and feel elastic rebound, a gentle bounce, not a crunch. Firm but friendly. Dense but not defiant. Try to pin it—nope, it glides sideways. Pain? Usually none. Heat? No. Drama? Only in your head. It’s doughy, it’s mobile, it’s annoyingly chill. Compare it to a stress ball that refuses to stress. You press, it yields, then returns. Repeat the test. Be skeptical. Be bold. Feel it move. Know the difference. Act with nerve.
Common Body Areas Where Lipomas Appear
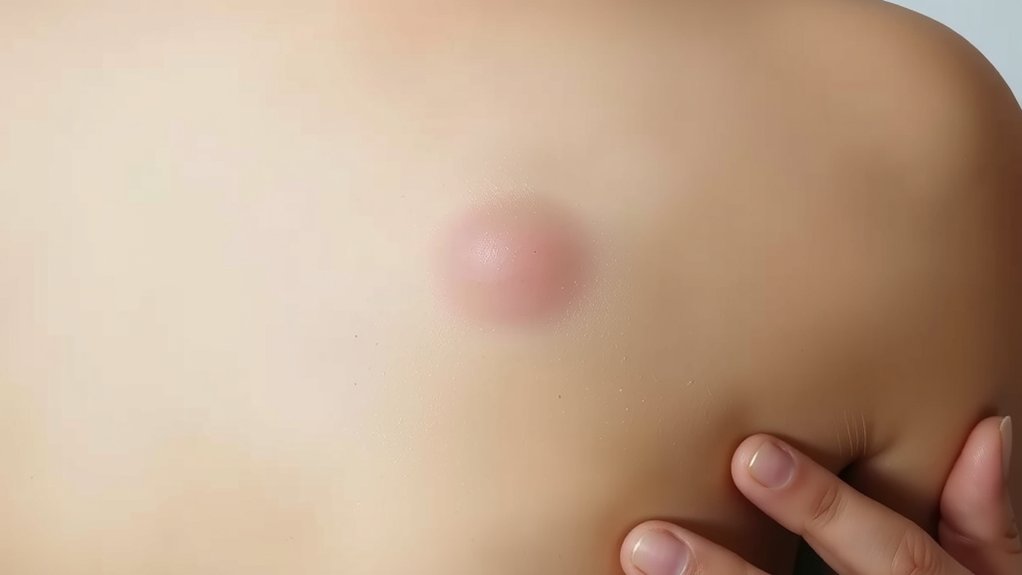
You think these lumps play hard to get—please. They love your trunk and shoulders, they hitch rides down your arms, they squat on your thighs, and they sneak up your neck. Feel bold; press, check, and call them out today—not tomorrow.
Trunk and Shoulders
Often, the first lump you notice parks itself on the trunk or shoulders—because of course it does. You run a hand across your back and there it is, soft, rubbery, sneaky. Not sharp. Not angry. Just stubborn. It slides a little under your skin when you push. You’d hate that. Good. Pay attention.
On the chest or along the shoulder blade, it shows as a slow bump under calm skin. No color drama. No heat. Boring, right? Until your backpack strap, sports bra, or seat belt grinds it daily. Then you’ll notice. You shift, you wince, you plan. Even your tattoo placement gets messed up; ink over a bulge looks warped, cruel mirror. Think about posture effects too. Posture shifts, pain follows, habit lies.
Arms, Thighs, Neck
Where do they show up next? Your arms. Of course. You flex, a soft lump rolls, and you pretend it’s nothing. It’s mobile, rubbery, smug. You poke it, it scoots. Annoying? Yes. Dangerous? Rarely. Then thighs. You sit, it squishes sideways like a lazy marshmallow. Pants rub it raw. So you make wardrobe adaptations, because apparently fabric negotiates now. Run a mile, it jiggles along, uninvited coach. And the neck. That’s where vanity screams. Collars scrape. Scarves argue. Sudden jewelry adjustments, because the chain keeps catching on your new “pearls.” You worry it’s cancer. It’s probably not. But you’re not guessing. You schedule the check. You demand answers. If it’s lipoma, fine. If not, better to know, today, not someday. Book it. Stop stalling.
Size, Shape, and Growth Patterns Over Time
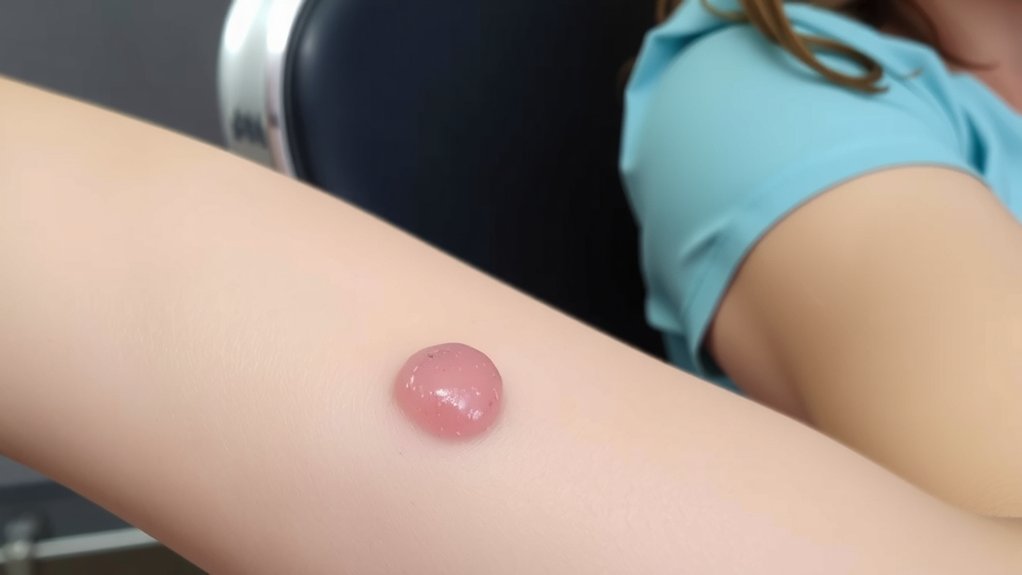
Although it sits quiet under your skin, size and shape shout the profile: lipomas are usually small—pea to plum—soft, rubbery, round or oval, and they slide when you push them.
Too firm? Too jagged? A lipoma feels lazy, like dough that won’t fight back. You press. It dodges. That mobility matters. Growth pattern? Slow. Months, years, not days. If it balloons fast, stop guessing; get it checked. Want numbers? Use a ruler, same angle, same pressure—measurement standards, not vibes. Log width and height, depth if a clinician measures. Then compare. Plot the changes. Statistical modeling for your squishy hitchhiker? Silly. Useful. Very, very true. Stable size wins. Creeping increases demand attention. Edges stay smooth. Skin stays normal. Pain stays minimal. Deviations shout. You listen.
Who Is Most Likely to Develop Lipomas
You think you’re safe at 16? Nice try—lipomas show up more after 40, and men edge women, though anyone can get the squishy surprise. Got relatives with soft lumps? Your odds spike—genes don’t ask permission. And certain syndromes and conditions stack the deck—Gardner syndrome, Dercum’s disease, Madelung’s—plus weight gain or metabolic chaos, so if that roster rings a bell, pay attention now.
Age and Gender Trends
Usually, lipomas crash the party in midlife—think 40 to 60—just when you thought your body had settled down. Surprise. You wake up, feel a squishy lump, and your brain yells nope. Age matters. Kids rarely get them. Teens almost never. You? Prime time. And gender? Reports wobble. Some clinics see a slight male edge. Others don’t. Translation—you’re not special. Anyone can join the club. Still, gendered stigma sticks to bodies. You’re told men should ignore bumps and women should hide them. Ridiculous. Those scripts warp your aging perceptions, make you delay care, make you worry more than you need. Lipomas grow slow, stay soft, mostly harmless. You check them. You name them. Then you move on. Because you run the show. Now act accordingly.
Family History Risk
When your family tree sprouts lumps, pay attention. Lipomas run in families more than you think. If your parent has soft squishy bumps, your odds jump. Not destiny. Just increased risk. You don’t wait for a surprise; you look. You ask blunt questions. That’s called family communication, not gossip. Who had bumps, where, how many, how fast. You write it down. Patterns matter. Privacy concerns? Sure. Respect them. But silence helps no one. Share only what you must, with people you trust. Check your shoulders, back, arms, thighs. Feel for mobile pads under skin. Small today, bigger tomorrow. Catch early, worry less. Don’t dramatize. Do notice. And if relatives shrug, push back. Your body, your call. You lead, they follow. Start now. Not later.
Associated Syndromes and Conditions
Family history is the smoke, but some fires come with names. If you’ve got Dercum’s disease, painful fatty nodules crash the party early and often. They burn, they bruise, they dare you to ignore them. Got Gardner syndrome? Expect lipomas alongside colon polyps, cysts, and bone bumps—like an overachieving troublemaker. Neurofibromatosis, Cowden, and Madelung’s mean more sparks. Metabolic chaos helps too: obesity, diabetes, rapid weight swings. Certain meds poke the bear. So do middle age and male bias, though women aren’t off the hook.
Here’s the punchline. Most lipomas are random. You didn’t earn them. But patterns matter. You see clusters, pain, growth, or family stacks? You see syndromes. Don’t wait. Photograph lumps. Map locations. Push for evaluation. Biopsy if doubt screams. Do it.
Lipoma vs. Cyst vs. Other Lumps: Key Differences
Why does that lump freak you out? Because names matter. Lipoma feels soft, doughy, and slides under your fingers. A cyst feels tense, like a grape with a peel; it may have a tiny pore. Other lumps? Nodes feel bean‑like and mobile; scars like dermatofibromas feel tethered. You want certainty. Fine. Think function. Lipoma = fat. Cyst = trapped gunk. Node = immune gear. Different origins, different behaviors. Histology differences seal it: mature adipocytes in lipoma, keratin‑filled sac in epidermoid cyst, lymphoid architecture in nodes. Imaging helps but hands talk first. You push. It glides. Probably fat. You press. It springs. Likely cyst. Money talk? Insurance implications vary by code: cosmetic removal versus symptomatic treatment. Guess wrong, pay twice. Choose wisely, not by panic.
Red Flags That Warrant Medical Evaluation
Although that lump might act harmless, some signs slam the brakes and say see a doctor now. If it explodes in size, you don’t wait. If it hurts, burns, or wakes you up, you move. Weakness, numbness, clumsiness? That’s neurologic deficits, not vibes. Fever, night sweats, weight loss—classic constitutional symptoms. Stop rationalizing. A rock‑hard mass that won’t budge, or one stuck deep, isn’t cute. Redness, heat, pus, foul smell—nope. Over joints, in the armpit, or pressing a nerve? Enough. Get checked.
| Red flag | Look | Why it matters |
|---|---|---|
| Rapid growth | Weeks, not months | Aggressive process possible |
| Persistent pain | Night pain | Inflammation or malignancy |
| Fixed, firm | Doesn’t slide | Deeper invasion risk |
| Skin changes | Red, hot, ulcer | Infection or necrosis |
Yes, you. Stop guessing. Call today now.
How Clinicians Diagnose a Suspected Lipoma
How do clinicians actually call the shot on that lump? They start with you, not the rumor. History first. When did it show up, did it grow, does it ache, what changed. Then hands on. They map size, depth, slip, borders. Soft like dough or stubborn like a rock. Mobile or glued. Honest clues.
Now the machines talk. Ultrasound Imaging checks if it’s fat, well circumscribed, non‑vascular. Fast. Safe. Cheap. If it looks weird or lives deep, they escalate with MRI, because shadows lie. Still not convinced? Fine. Needle Biopsy. A small poke. Cells tell the truth, not your hopes. Pathology rules, period.
You want certainty, right? Then let the process work. Bring facts. Ditch guesses. Answer straight. Stop stalling. Schedule the exam now.
Treatment and Removal Options
Ready to deal with the lump or keep pretending it isn’t there? You’ve stared at it long enough. It’s soft, smug, and not paying rent. Two main plays. Surgical excision—clean cut, out it goes, specimen bag, goodbye. You want definitive? That’s it. Small scar, big relief. Or liposuction removal—tiny slit, cannula, fat confetti, faster bounce back. You like minimal drama? Pick that. But don’t kid yourself. Big, deep, or awkward spots often demand the knife. Pain? Brief. Numbing helps. Downtime? Days, not doom. Risks? Bleeding, infection, recurrence—rare, not mythical. You still hesitating? Why let a pillow of fat run your schedule. Get a consult. Ask costs, scars, time off. Choose. Commit. Stop doom‑scrolling. Start fixing. Yes, today. Your move, not the lump’s, make it.