What does a PE feel like? Like your chest stabbed you every time you breathe. Like you walked five steps and ran a marathon. Your heart sprints, your head swims, maybe you cough up blood—fun, right? Or it’s sneakier: one calf swells, aches, feels hot, and you shrug it off. Don’t. This isn’t “I’ll wait it out.” It’s now. Because the gap between brush‑off and blackout is minutes—and here’s how to tell.
Key Takeaways
- Sudden, unexplained shortness of breath that doesn’t improve with rest, often feeling like air is scarce.
- Sharp, stabbing chest pain that worsens with deep breaths or coughing (pleuritic pain).
- Rapid heartbeat, sweating, dizziness, or a sense of panic; sometimes inability to lie flat.
- Persistent cough that may produce blood-streaked sputum, plus unexplained fatigue or palpitations.
- One-sided calf swelling, warmth, and tenderness may precede chest symptoms and suggests a leg clot source.
Common Warning Signs in the Chest and Lungs

When a clot parks itself in your lung, your chest won’t whisper—it yells. You feel a stab when you breathe. Sharp. Mean. Like a knife under the ribs that hates you back. Air gets scarce fast, and you gasp, because pride can’t beat physics. You cough, again and again, a persistent cough that won’t take a hint. Maybe you spit red streaks—bloody sputum, not drama. Your heart sprints like it heard a starting gun. You sweat. You sit up, then you pace, then you swear. Lying flat? Feels like drowning. Deep breath? Nice try. It burns. You grab the railing. You want out of your own body. So move. Call now. Don’t negotiate with pain. Don’t wait for permission. Get help. Prove you’re stubborn.
Subtle Symptoms That Are Easy to Miss

Usually it doesn’t roar. It whispers, then shrugs. You feel off, not dying, just wrong. You blame Mondays, coffee, screens. Smart. Meanwhile a clot plays hide‑and‑seek. Breath seems fine until stairs turn brutal. You stop, pretend to check your phone, and bargain with air.
Your body throws small flags. Mild fatigue that lingers like gum under a desk. Intermittent dizziness when you stand, then you laugh it off, because superheroes don’t wobble. A fluttering heartbeat that speeds for no polite reason. A sweat that shows up indoors in January. Tiny coughs that refuse a plot twist. Anxiety out of nowhere, sharp and bossy.
You want a rule? Simple. If your normal feels hijacked and keeps returning, don’t debate it. Call, get checked, win oxygen.
Leg Clues: DVT Symptoms That Precede a PE
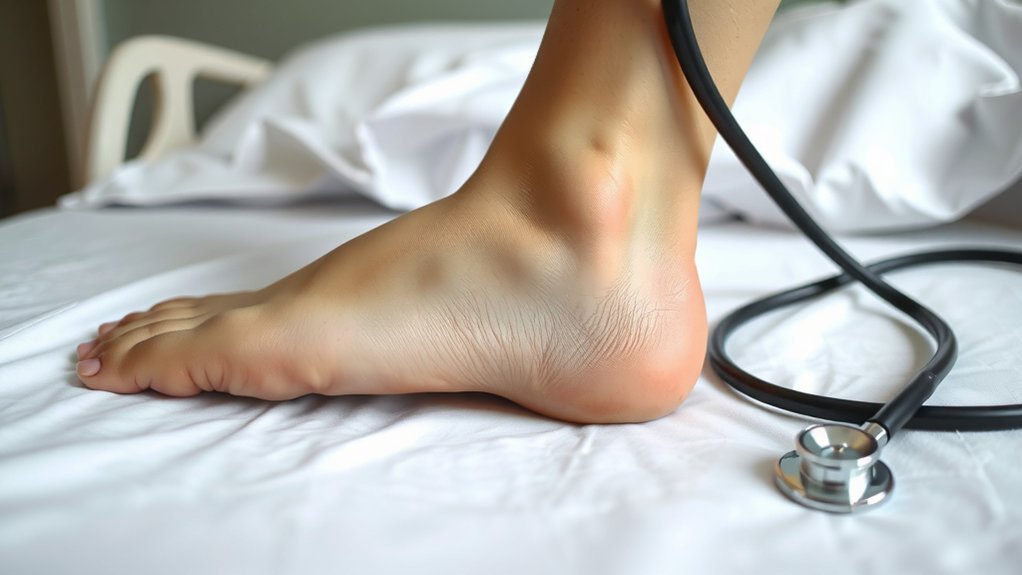
You spot one leg puffing up while the other looks normal—yeah, that lopsided balloon isn’t cute, it’s a warning. Your calf screams when you walk and flinches at a light squeeze, and you still want to shrug it off? Stop calling it “just a cramp”; call a clinician now before that clot takes the express to your lungs.
Unilateral Leg Swelling
Although it might look like a gym win, one leg swelling bigger than the other is a red flag, not a flex. Your jeans fight one calf. Your sock leaves a trench. The skin feels tight, hot, shiny. That’s not gains. That’s a warning.
Unilateral swelling screams mismatch. Blood isn’t draining right. A clot can choke the flow and set you up for a pulmonary embolism. Yes, the big, deadly kind. Not tomorrow. Now. Call it out. Get checked.
Could it be something else? Sure. Sprain, Lymphedema causes, Medication reactions, long flights, salt binges. But DVT sits high on the list, and you don’t get style points for guessing wrong.
Measure both legs. Notice sudden change. Don’t massage. Don’t wait. Seek urgent care. Today.
Calf Pain and Tenderness
How does a clot announce itself? With calf pain that nags, then bites. You stand up, it stabs. You walk, it burns. Touch the calf—tender, tight, wrong. Not a cute cramp. Not your classic muscle strain from weekend heroics. It hurts at rest. It hates when you flex your ankle. It may swell, feel warm, look angry. And no, rubbing it won’t fix it. Press and it protests. Pull your toes up and it curses you. That’s a red flag. Keep marching and you gamble big—pieces can break, fly north, and choke your lungs. Still think it’s nothing? Fine, roll those dice. But if pain escalates, or the leg turns hard, woodlike, think compartment syndrome, think emergency. Call. Now. Don’t negotiate with clots. Today.
How PE Symptoms Differ From Heart Attack, Asthma, or Panic

You love guessing games with chest pain—bad idea. In PE, the pain hits sharp and stabbing, worse when you breathe deep or cough, not the crushing squeeze that crawls down your left arm like a heart attack. Breathless out of nowhere while sitting on a plane or after lazy days—that screams PE; asthma wheezes and calms with an inhaler, panic hammers fast breathing and fades when you slow it down, so match the trigger and the feel or get burned.
Chest Pain Characteristics
When chest pain hits, the pattern matters more than the panic. You want answers, not platitudes. With a pulmonary embolism, the pain quality is knife-sharp, one-sided, and mean. It stabs when you move, it refuses massage, and it doesn’t fade because you wish it away. Pain intensity spikes fast, then lingers like a bad idea. Heart attack? Different beast. Heavy, crushing, center stage, marching to the jaw or left arm like it paid for VIP. Asthma feels like a tight band squeezing the ribs, persistent, bossy, not pokey. Panic loves drama—zippy, shifting, hot and cold, here then gone, then back—because your brain’s playing DJ. Press your chest. If touch recreates it, think muscle. If nothing changes, don’t flex. Pay attention. Act now today. Seriously.
Breathlessness and Triggers
Even if you blame it on a long day, PE breathlessness doesn’t care—it slams in fast, out of nowhere, and sticks like glue. You stop. You grab air like it owes you money. It doesn’t ease when you sit. It laughs at rest. Climb two steps and feel wrecked. No warm up. No mercy.
Asthma? Triggers like air pollution, high humidity, dust, exercise. Inhaler helps. Pattern shows up. Panic? Chest tight, mind racing, but breathing deep eventually lands. You can talk through it. Heart attack? Heavy, crushing, spreading to arm or jaw. Slow down and it still screams.
PE says move or sit, same punishment. Sharp breaths. Rapid pulse. Maybe cough, maybe blood. Scary sudden. Feels wrong. Trust that alarm. Don’t stall. Act now.
Who Is at Higher Risk for a PE
Although PE can blindside anyone, some people carry a loaded deck. You know if that’s you. Family clots? That’s a flashing siren called Genetic thrombophilia. You sit for hours, you fly, you game, you heal after surgery—blood pools, trouble brews. Hormone therapy, pregnancy, or postpartum? Estrogen turns the dial up. Cancer does too. So does smoking. Extra weight piles on risk. Age isn’t kind. Prior DVT or PE? You’re already marked.
| Higher risk | Why it bites |
|---|---|
| Major surgery or long immobilization | Blood stagnates then clots |
| Hormone therapy, pregnancy, postpartum | Estrogen boosts clotting |
| Genetic thrombophilia, family history | You clot faster than others |
Don’t wait for luck. Ask your doctor. Move more. Hydrate. Ditch cigarettes. Plan breaks on trips. Spot swelling or pain. Act. Later. Now.
What PE Feels Like During Activity vs. At Rest
Risk is one thing; the hit is another. During activity, a PE feels like the air rebels. You push and your chest tightens like a vise. Breath turns thin. Steps shrink. That sudden wall? That’s exercise limitation, not laziness. Your heart hammers rude and fast, yet the legs burn cold. You pause, it doesn’t reset. Stairs look taller. Jokes aren’t funny because laughing steals oxygen. Sharp stabs may tag each inhale, mean little jabs that boss you around. At rest, it doesn’t play nice either. You feel heavy, dull, alert and exhausted. Quiet room, loud lungs. Resting fatigue drapes over you like wet cloth. You sigh a lot. You sit still and still feel chased. Calm body, panicked breath. Wrong, and you know it.
When Symptoms Mean You Should Seek Urgent Care
How do you know it’s time to stop guessing and go now? When your chest feels like a closing fist, when breath slices short, when you’re dizzy or coughing blood. Not later. Now. Sudden worse pain with a deep breath? Calf tight, hot, swollen? Sit down. Call. Don’t crowdsource survival.
| Red flag | Do this |
|---|---|
| Crushing chest pain, gasping, fainting | Call 911; don’t drive |
| New leg swelling plus sharp chest pain | Stop, breathe, give location |
Use emergency contacts on speed dial. If alone, speakerphone. Doors unlatched. Pets contained. No hero stunts. Ambulance beats DIY transport options. Why? Monitors, meds, oxygen. Your car has none. Debating costs while your oxygen drops is… bold. Pick life. If you’re wrong, you’re alive. If you wait, you might not.
What to Expect During Evaluation and Diagnosis
So what happens when you hit the ER doors? Nurses grab readings. You gasp. They move. You get oxygen, IV, monitors. No small talk. Straight to questions: chest pain, leg swelling, travel, hormones, surgery. Answer fast. Guessing kills.
Then the Lab tests hit. D‑dimer if risk seems low. Troponin, BNP, blood gases if things look ugly. Numbers don’t lie, but they don’t finish the story.
Next comes the Imaging process. Chest CT with contrast, loud, fast, decisive. You hold breath. Scanner hunts clots. Can’t do contrast? Fine. V/Q scan steps in, old school but sharp. Legs sore? Ultrasound hunts DVT like a sniffer dog.
While you wait, they start blood thinners. Not later. Now. Because clot time is bully time. It doesn’t wait. Ever.